By Dr. Vishal Anand, Healthcare BA and Vikram Suthankar, Asst. Vice President & Consulting Head, Healthcare Providers
The emergence of provider-led health plans (Payviders) is an excellent opportunity for provider systems to break the payer-provider silos and improve value-based care. Although, the convergence between payers and providers had led to better decision-making abilities and reduced financial risk sharing, there are opportunities for Payviders to deliver better consumer value and ensure fair margins.
In this five-part blog series, we will be highlighting key technology areas – data integration & interoperability, data curation & management, performance analytics, data science & digital innovation, and core workflows & applications – that would enable Payviders to drive value chain excellence.
Interoperability Trends & Challenges for Payviders
Industry Trends
1. CMS IPA Rule
The CMS IPA rule aims to empower members and patients by providing access to their health data and increase interoperability among payers, providers and patients. Recent additions such as pre-authorization to the existing rules have made it mandatory for Payviders to have best in class interoperability solutions.
2. Industry Initiatives
Healthcare companies from the private sector formed initiatives such as the Da Vinci Project and CARIN for Blue Button Framework to simplify member engagement and care coordination. Some of the member access use cases include clinical data exchange, payer data exchange, directory, formulary, payer coverage decision exchange, and price cost transparency.
3. COVID-19 Pandemic
The COVID-19 crisis has further put the focus on the importance of interoperability for health plans including Payviders. Many healthcare organizations are collaborating to form a Vaccination Credential Initiative (VCI) to establish a standard for digital vaccination records. The VCI will enable organizations administering COVID-19 vaccines to make credentials available in a standardized and interoperable format. The new system uses SMART health cards framework based on HL7 FHIR standards.
4. Emerging Forms and Sources of Data
Patient generated health data (PGHD) obtained from Internet of Medical Things (IoMT) devices such as wearables, home monitoring devices, etc. is helping Payviders implement remote patient monitoring use cases and leverage IoMT and standards such as FHIR for going beyond population health to personalized healthcare and precision medicine.
Health plans have also started leveraging social determinants of health (SDoH) data to enrich clinical and claims data for holistic member engagement and health management. Social media data mining for healthcare can complement other data sources for identifying and analyzing behavioral patterns.
Key Challenges
1. Inconsistent Adoption of Standards
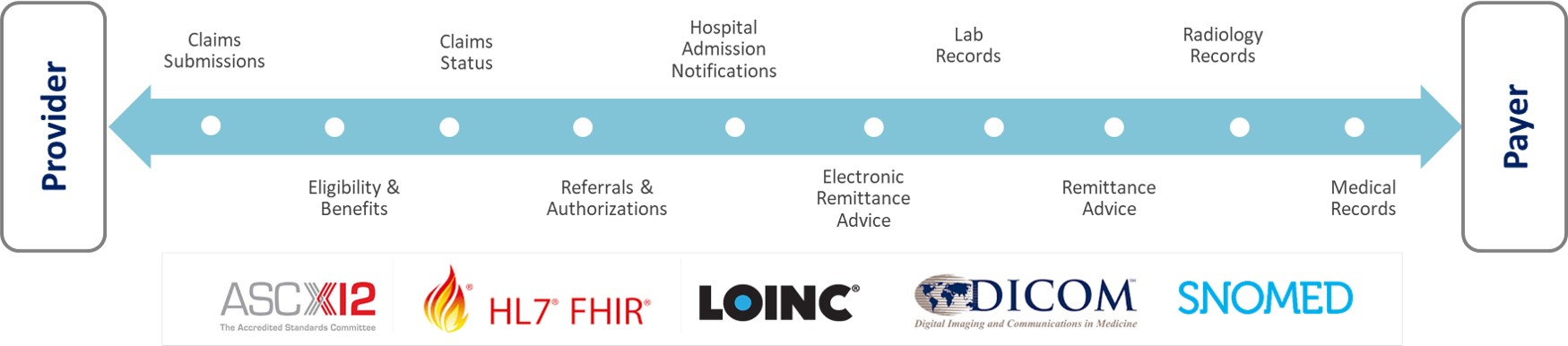
Multiple source systems and data transfer between different payer systems, EHR systems, 3rd party applications, different medical devices, wearables and social media, portals, and mobile applications often result in inconsistencies in data standards. Although there are standards in place (X12, HL7, DICOM, LOINC, SNOMED, etc.), the implementation of these standards is subjective and inconsistent, making it difficult to integrate, curate, and operationalize data while ensuring compliance to regulatory requirements.
- Unstructured Data
Unstructured data from EOBs (explanation of benefits), patient charts, clinical notes, radiology images, etc. make it extremely difficult for health plans to interpret and standardize, and derive insights in a meaningful manner.
- Privacy and Security
With exchange of huge volume of data across multiple systems and applications, the privacy and security of healthcare data shared is at an increased risk and subject to various phishing and other cyber-attacks. Despite interoperability’s ability to provide improved patient data access to providers and members, it may also create an increase in healthcare data breach risk.
Solution Considerations
- Data Integration
Payvider organizations need a comprehensive data management solution that can integrate and curate data from a diverse set of healthcare applications, establishing an enterprise’s data architecture. Organizations should have a data lake where all categories of corporate data can be stored for a wide variety of data distribution use cases.
A modern integration / interface engine is crucial for all Payvider organizations to facilitate the exchange of clinical, financial and operational data across healthcare systems. Organizations could also opt for an Integrated Platform as a Service(iPaaS), a cloud-based solution as it supports real time integration and effectively manages high volume of mobile, ETL and EDI data.
Organizations should work towards to create safe, secured, and consumable APIs. It would allow exposure of APIs in a safe and secured way to 3rd party applications for developer use.
Usage of NLP accelerators is also very important for Payviders. Clinical information is primarily generated from unstructured formats like clinician notes, voice or images, which are beneficial if extracted properly. NLP accelerators help fetch useful data from these unstructured formats and sources, making the data structures comprehensible.
- Data Interoperability
The FHIR standard is being adopted by large health systems and health plans, encouraging the industry to adopt a uniform standard of interoperability. FHIR based applications enable patients / members to access all the information available ranging from preventive care checks to status of outstanding claims.
Organizations should have a strong foundation in integrating and sharing data in FHIR formats by leveraging components such as FHIR mapper, FHIR parsers, FHIR repository, FHIR Façade, FHIR API, etc.
Data sharing security and privacy concerns can be addressed by establishing a robust authorization & authentication mechanism with OAuth 2.0 framework and consent management features to ensure healthcare data protection.
SMART-on-FHIR has started to receive industry wide adoption and presents significant opportunities for developing intuitive and workflow-integrated applications for payers, providers, and members for effective care coordination and secure information sharing.
- Heath Information Exchanges
HIEs and Regional Health Information Organizations (RHIOs) play a significant role in allowing secure, easy, timely and precise exchange of healthcare data among patients, providers, health plans, ACOs, etc. There are several national and state level initiatives such as SHIEC, PCDH, etc. that continue to evolve the role of HIEs to drive better care coordination and health outcomes across providers, payers and ACOs. While HIEs have traditionally been a great source of clinical data, few states are also implementing All-payer Claims Databases (APCDs) to holistically manage quality and cost of care and conform with evolving value-based payment reforms.
Data integration is one of the most critical areas to truly drive Payvider value chain excellence. The advances in technology and healthcare standards along with regulations such as the CMS IPA rule are making it imperative for Payviders to adopt and create a more interoperable and efficient ecosystem and drive healthcare and business outcomes.




